What is Anterior Interbody Fusion in Spine Surgery?
Anterior interbody fusion (AIF) is a vital technique in modern spine surgery. Dr. John Smith, a renowned spine surgeon, states, "Anterior interbody fusion can significantly enhance stability and reduce pain." His expertise underscores the importance of this procedure.
In AIF, surgeons remove damaged discs and insert bone grafts to fuse vertebrae. This method promotes effective healing and restores spinal alignment. Many patients report lower pain levels after surgery. However, the approach has its challenges. Complications can arise, and not every patient responds positively.
While AIF shows promise, it’s not a one-size-fits-all solution. Selecting appropriate candidates is critical. Long-term effectiveness varies among individuals. Continuous research and surgeon experience are essential for refining AIF techniques and improving patient outcomes.
Definition and Overview of Anterior Interbody Fusion
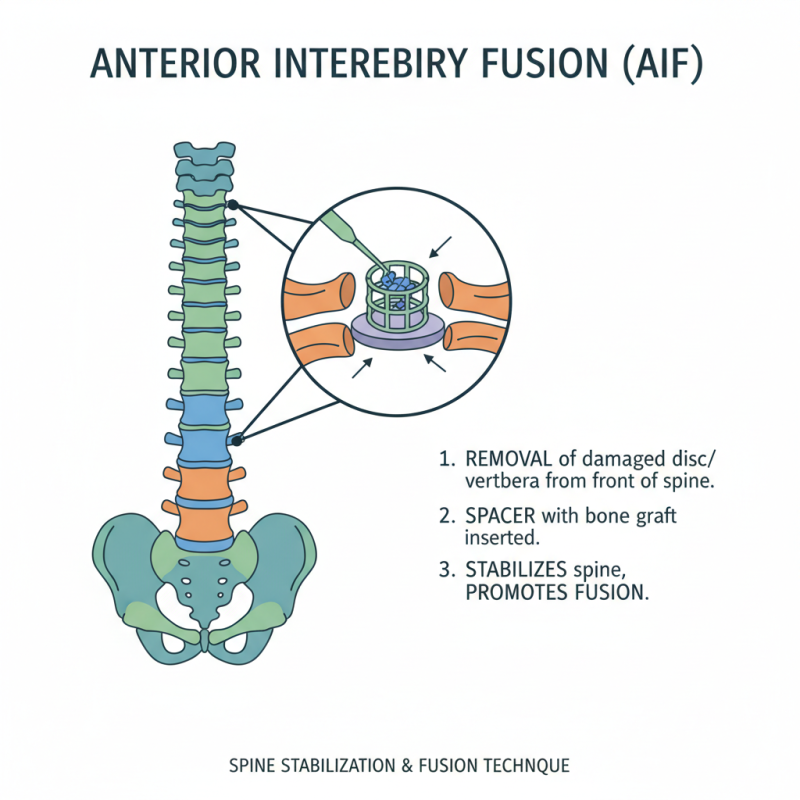
Anterior interbody fusion (AIF) is a surgical technique used in spine surgery. It involves the removal of a damaged disc or vertebra from the front of the spine. Once this is done, a spacer filled with bone graft or a similar material is inserted into the disc space. This method aims to stabilize the spine while promoting fusion between adjacent vertebrae.
The AIF procedure offers several advantages. It provides direct access to the spinal column, minimizing tissue damage. Patients may experience faster recovery times and less pain compared to posterior approaches. However, it is not without risks. Complications can occur, such as nerve damage or infection. Surgeons must take care to evaluate each patient thoroughly. Not every candidate will benefit from this technique.
Post-operative success relies on proper patient selection and adherence to rehabilitation protocols. Some may struggle with pain management or mobility after surgery. These factors deserve careful consideration during planning. Patients should participate actively in their recovery process. Open communication with healthcare providers is crucial for optimal outcomes.
Indications for Anterior Interbody Fusion in Spine Surgery
Anterior Interbody Fusion (AIF) is a common technique in spine surgery. It is often employed for various spinal conditions. This method is particularly beneficial for patients suffering from degenerative disc disease, spondylolisthesis, or spinal instability. According to a report from the American Academy of Orthopaedic Surgeons, over 400,000 spinal fusion surgeries are performed annually in the U.S. alone.
Indications for AIF include severe back pain not relieved by non-surgical treatments. Patients with substantial nerve compression also qualify for the procedure. The goal is to stabilize the spine and relieve pain. Studies show that AIF can lead to significant improvement in patient-reported outcomes, with a fusion success rate reported between 80% and 90%. However, not all patients respond positively. Complications can arise, such as infections or nonunion of the fusion.
It is crucial to choose AIF for appropriate candidates. A thorough evaluation is needed to assess the patient's condition and lifestyle. Not every patient with back pain is suited for surgery. A multi-disciplinary approach often yields the best results. Engaging in pre-operative discussions helps to set realistic expectations for recovery and outcomes. Data on long-term efficacy is still evolving, and more research is required to determine disparity in success across diverse patient populations.
Indications for Anterior Interbody Fusion in Spine Surgery
This bar chart illustrates the common indications for anterior interbody fusion in spine surgery, highlighting the percentage representation of each indication based on recent surgical data.
Surgical Techniques and Procedures in Anterior Interbody Fusion
Anterior Interbody Fusion (AIF) is a common technique in spine surgery. This approach focuses on accessing the spine from the front, allowing for a clear view of the intervertebral disc space. The procedure involves removing the damaged disc, which may be contributing to pain or instability. Surgeons then place a fusion cage or bone graft to promote healing and stability.
One key advantage of AIF is reduced muscle disruption compared to traditional posterior approaches. According to a study published in the "Journal of Spinal Disorders & Techniques," patients often experience less postoperative pain and faster recovery times. AIF can provide better alignment for the spine, which is crucial for long-term outcomes. However, the technique also has challenges, such as potential damage to abdominal organs during access.
Tip: Before considering AIF, discuss all risks with your surgeon. They can provide valuable insights based on their expertise.
A comprehensive understanding of AIF is essential for both patients and medical professionals. The procedure requires not just technical skills but a thorough evaluation of each patient’s unique situation. For instance, a study in the "Spine Journal" highlights that while AIF has a success rate of about 80-90%, patient selection plays a pivotal role in outcomes. Some individuals may face complications, such as nonunion or infection, underscoring the need for clear communication and tailored care.
Tip: Always seek a second opinion to ensure that AIF is the right choice for your condition.
Risks and Complications Associated with Anterior Interbody Fusion
Anterior interbody fusion (AIF) is a common approach in spine surgery. This technique does carry risks and complications that patients should be aware of. According to a study published in the Journal of Bone and Joint Surgery, complications can occur in up to 20% of cases. These may include infection, bleeding, and nerve damage.
One concerning risk is adjacent segment disease. This can develop in nearly 25% of patients who have undergone fusion. Such complications often require additional surgeries. Patients should discuss these risks with their surgeons, as understanding is key.
Tips: Stay active pre-surgery. Increased strength can aid recovery. Also, seek a second opinion. Different surgeons may offer varied insights into potential risks.
Proper patient selection is vital. Some individuals may not be suitable candidates for AIF due to pre-existing conditions. This could lead to poor outcomes. Always assess individual risks before proceeding. It's crucial to weigh the benefits against these potential complications for informed decision-making.
What is Anterior Interbody Fusion in Spine Surgery? - Risks and Complications Associated with Anterior Interbody Fusion
| Aspect | Details |
|---|---|
| Definition | A surgical procedure that involves fusing two or more vertebrae through the anterior (front) part of the spine. |
| Indications | Conditions such as degenerative disc disease, spinal instability, or spinal fractures. |
| Risks | Infection, blood clots, nerve damage, or an adverse reaction to anesthesia. |
| Complications | Non-union of vertebrae, adjacent segment degeneration, or hardware failure. |
| Recovery Time | Typically 6 to 12 weeks, depending on individual patient factors and extent of surgery. |
| Success Rate | Generally reported between 80% to 90%, depending on the underlying condition and patient health. |
| Alternatives | Posterior lumbar interbody fusion, artificial disc replacement, or non-surgical options such as physiotherapy. |
Postoperative Care and Rehabilitation after Anterior Interbody Fusion

Postoperative care after anterior interbody fusion (AIF) is crucial for recovery. Patients often face challenges, such as managing pain effectively. A properly outlined pain management plan can help. Physical therapists may introduce gentle movements early on. Gradually increasing activity is vital for regaining strength.
Monitoring the surgical site is important. Keep an eye out for signs of infection, like excessive redness or drainage. Such issues can lead to complications. Patients should also be cautious about their posture and movements. Lifting heavy objects too soon can strain the surgical area. Proper body mechanics can prevent unnecessary stress on healing tissues.
Nutrition plays a key role in healing. A balanced diet rich in protein supports tissue repair. Hydration is equally important. Weakness and fatigue are common in the early weeks post-surgery. Patients must listen to their bodies and rest when needed. Reflecting on setbacks, like increased pain or slow progress, can be beneficial. Adjusting expectations helps in the journey to recovery.