Why Choose Lateral Interbody Fusion for Spinal Surgery?
Lateral interbody fusion has emerged as a leading technique in spinal surgery, offering unique benefits. A report from the North American Spine Society indicates that lateral interbody fusion procedures can lead to quicker recovery times and reduced complication rates. Dr. Vanessa Miller, a renowned spine surgeon, states, “Lateral interbody fusion minimizes the risks associated with traditional approaches while promoting better patient outcomes.”
The lateral interbody fusion technique allows for direct access to the spine, enhancing visualization. This minimally invasive approach reduces muscle damage and ensures faster rehabilitation. According to a study published in the Journal of Spine Surgery, patients who underwent lateral interbody fusion experienced a 30% improvement in postoperative mobility compared to those who had traditional procedures.
However, it's essential to consider that not every patient is ideal for this method. There can be challenges during the procedure, and not all surgeons are familiar with the technique. Continuous training and experience are critical. Overall, lateral interbody fusion represents a significant advancement in spinal surgery, yet it necessitates careful consideration and expertise for optimal results.
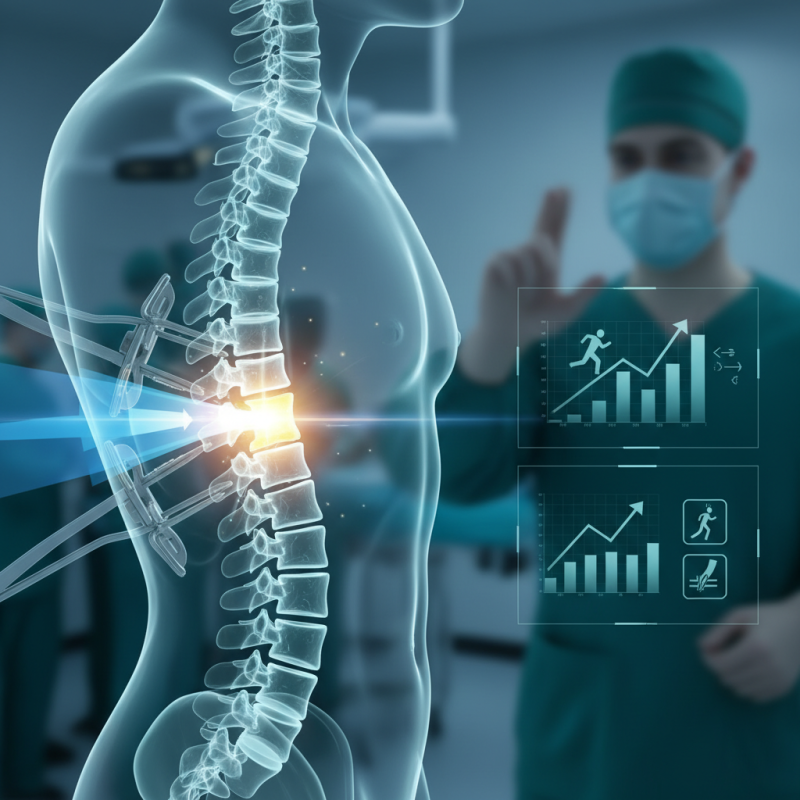
Understanding Lateral Interbody Fusion: An Overview of the Technique
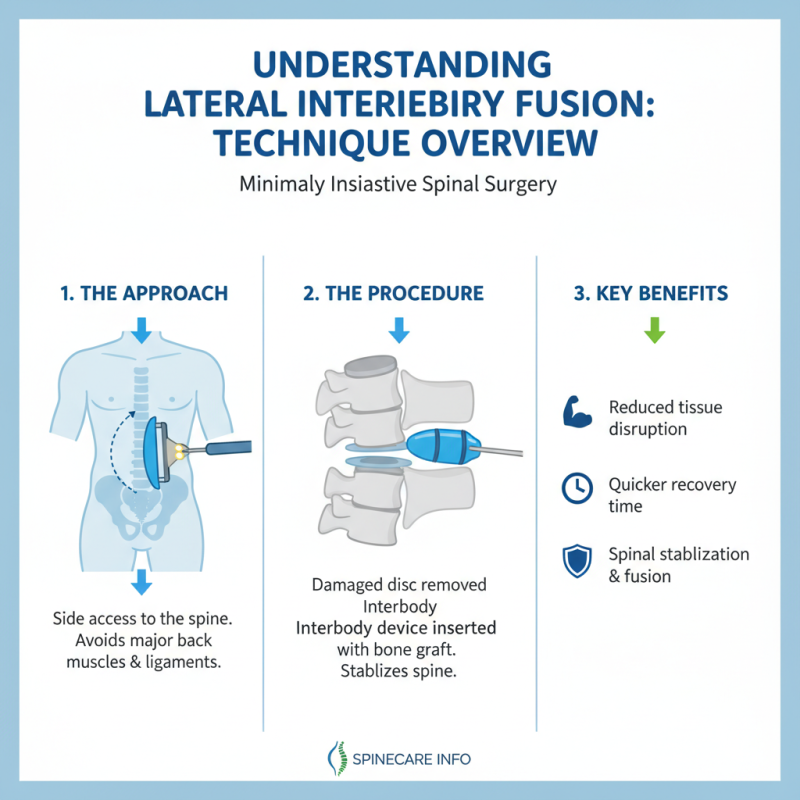
Lateral interbody fusion (LIF) is a minimally invasive surgical technique used in spinal surgery. This procedure accesses the spine from the side, rather than the back. It allows surgeons to avoid major muscles and ligaments. The approach minimizes disruption to surrounding tissues, leading to quicker recovery times.
During the procedure, the surgeon inserts a device between two vertebrae to support the spine. This device promotes bone growth, helping to fuse the vertebrae together. Surgeons can use imaging technology for precise placement. This enhances surgical accuracy and reduces complications. However, the learning curve for this technique can be steep. Not all surgeons may have the same level of expertise, which can affect outcomes.
Post-operative care is crucial. Patients must follow specific guidelines to ensure proper healing. Some may experience discomfort as they adjust to their new spinal alignment. It's essential to recognize that not every patient will have the same experience. Monitoring recovery closely allows for better management of any issues that arise. This reflects the complexity of spinal surgeries and the importance of individualized care.
Advantages of Lateral Interbody Fusion Compared to Traditional Methods
Lateral Interbody Fusion (LIF) offers distinct advantages over traditional spinal fusion techniques. This minimally invasive approach allows surgeons to access the spine through the side, reducing muscle disruption. A report by the American Academy of Orthopaedic Surgeons states that LIF can lead to significantly less postoperative pain. Patients often experience quicker recovery times and shorter hospital stays.
Research indicates that LIF has a lower complication rate compared to anterior or posterior spinal fusions. A study published in the Journal of Spine Surgery highlighted that LIF's overall complication rate was approximately 4%, significantly lower than the 10% to 15% seen in traditional methods. These findings suggest that patients opting for LIF can benefit from a more reliable surgical experience.
Despite these advantages, not all patients are ideal candidates for LIF. Factors such as obesity, severe spinal deformities, and previous surgeries may limit its effectiveness. Surgeons must evaluate each case carefully to ensure optimal outcomes. Balancing these considerations is essential for both patient safety and surgical success.
Why Choose Lateral Interbody Fusion for Spinal Surgery? - Advantages of Lateral Interbody Fusion Compared to Traditional Methods
| Aspect | Lateral Interbody Fusion | Traditional Methods |
|---|---|---|
| Surgical Approach | Minimally invasive from the side | Open surgery from the back |
| Muscle Damage | Less muscle damage | Significant muscle disruption |
| Recovery Time | Faster recovery | Longer recovery period |
| Hospital Stay | Shorter hospital stay | Longer hospitalization |
| Complication Rate | Lower complication rates | Higher complication rates |
| Patient Feedback | Higher satisfaction | Variable satisfaction |
Indications for Choosing Lateral Interbody Fusion in Spinal Disorders
Lateral interbody fusion (LIF) is a surgical technique gaining traction for treating various spinal disorders. This approach is often recommended for patients with degenerative disc disease, scoliosis, and spinal stenosis. Studies show that about 30% of patients suffering from these conditions may benefit from LIF due to its minimally invasive nature. It allows direct access to the spine while reducing trauma to surrounding muscles.
One notable advantage of LIF is its enhanced fusion rate. According to a report by the North American Spine Society, fusion rates for LIF can reach up to 94%, compared to traditional posterior techniques. This can lead to quicker recovery times, with patients often resuming normal activities within weeks rather than months. However, not every candidate is ideal for LIF. Factors like obesity, previous surgeries, or complex spinal deformities may complicate outcomes.
Complications can also arise, as is the case with any surgical procedure. A rapid review indicated that up to 15% of patients might experience some form of complication. These can include nerve injury or dissatisfaction with pain relief. Surgeons must weigh these risks against potential benefits when recommending LIF. Informed discussions between patients and clinicians are essential for making the right choice.
The Surgical Process of Lateral Interbody Fusion Explained
Lateral interbody fusion (LIF) is an innovative approach in spinal surgery. It involves accessing the spine from the side rather than the back. This method can reduce muscle damage and recovery time. The lateral position allows for better visualization of the spine, minimizing complications.
During the surgical process, the patient lies on their side. The surgeon makes a small incision on the side of the abdomen. Specialized instruments help to gently navigate through the muscles and tissues. Once the spine is accessed, any damaged discs can be removed. The surgeon inserts a spacer to maintain proper alignment and stability.
Post-surgery, patients often experience less pain and quicker rehabilitation. However, challenges can arise. Not all patients are suitable candidates for LIF. Surgeons must carefully evaluate individual cases. Some may find the recovery more difficult than expected. Each surgery should be approached with thorough consideration of risks and benefits. The journey of recovery requires patience and commitment.
Lateral Interbody Fusion Advantages Over Traditional Approaches
This chart highlights the perceived advantages of Lateral Interbody Fusion (LIF) compared to traditional spinal fusion methods based on various criteria, including recovery time, hospital stay, and pain levels.
Postoperative Care and Recovery Following Lateral Interbody Fusion Surgery
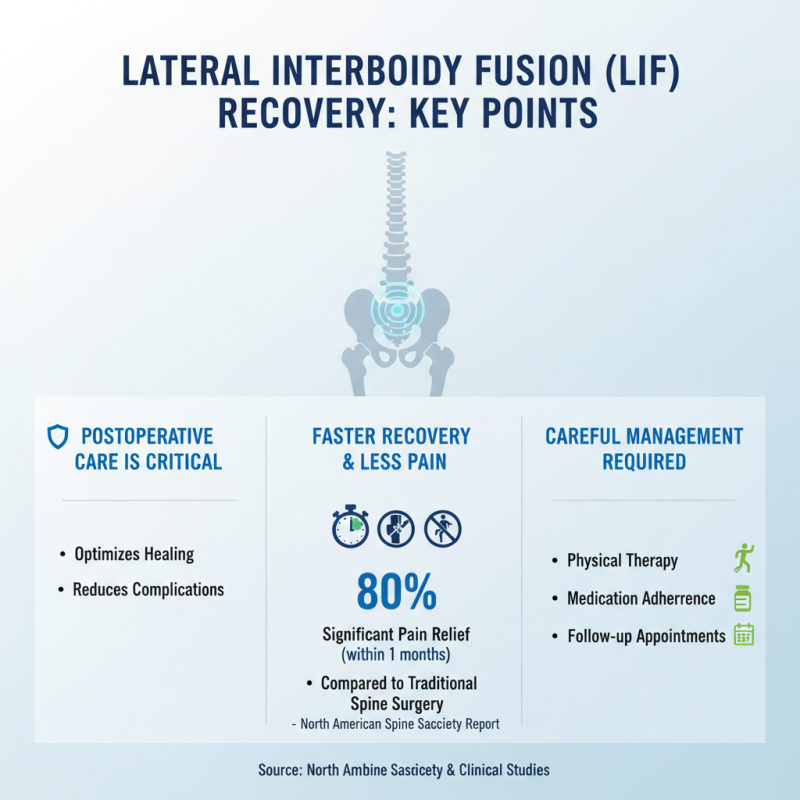
Postoperative care following lateral interbody fusion (LIF) is critical for optimal recovery. Studies show that patients often experience less pain and faster recovery times with LIF compared to traditional approaches. A report from the North American Spine Society highlights that approximately 80% of patients achieve significant pain relief within six months. However, the recovery process requires careful management.
After surgery, patients typically stay in the hospital for 1 to 3 days. During this time, monitoring for complications is vital. Common issues include infection and nerve damage, which can occur in about 1% of cases. Physical therapy usually starts within 24 to 48 hours post-surgery. Engaging in gentle movements can promote healing but also requires caution. Patients should avoid high-impact activities for several weeks.
At home, adherence to a prescribed pain management plan is crucial. Many patients may underestimate their need for rest and may push themselves too quickly, leading to setbacks. Regular follow-up appointments help track progress. According to a study in the Journal of Neurosurgery, about 10% of patients report prolonged recovery, signifying that individualized care is essential. Understanding these factors can significantly enhance patient outcomes.
Related Posts
-

What is Lateral Interbody Fusion at the 139th Canton Fair?
-
10 Best Techniques for Posterior Lumbar Interbody Fusion?
-

Discover the Best ASC Solutions for China Top Suppliers?
-
What is Anterior Interbody Fusion in Spine Surgery?
-

How to Choose the Right Screw System for Your Project?
-

Top 10 Surgical Surgeons in China You Should Know About?
