Top 10 Cervical Fixation Techniques You Need to Know?
Cervical fixation techniques are crucial in spinal surgeries. These procedures stabilize the cervical spine and promote healing. Dr. Emily Carter, a renowned neurosurgeon, states, “Effective cervical fixation can drastically enhance patient outcomes.” This highlights the importance of understanding various fixation methods.
Choosing the right technique for cervical fixation can be complex. Each method has unique benefits and challenges. Surgeons must assess patient needs carefully. Some traditional methods may be familiar, while newer techniques can offer improved results. It is essential to stay updated with innovations in this field.
As we explore the top 10 cervical fixation techniques, it’s vital to recognize both their strengths and potential drawbacks. No technique is perfect, and missteps can occur. Surgery often involves uncertainties. Understanding these nuances is key for optimal patient care. This overview aims to enlighten both patients and practitioners about effective cervical fixation options.
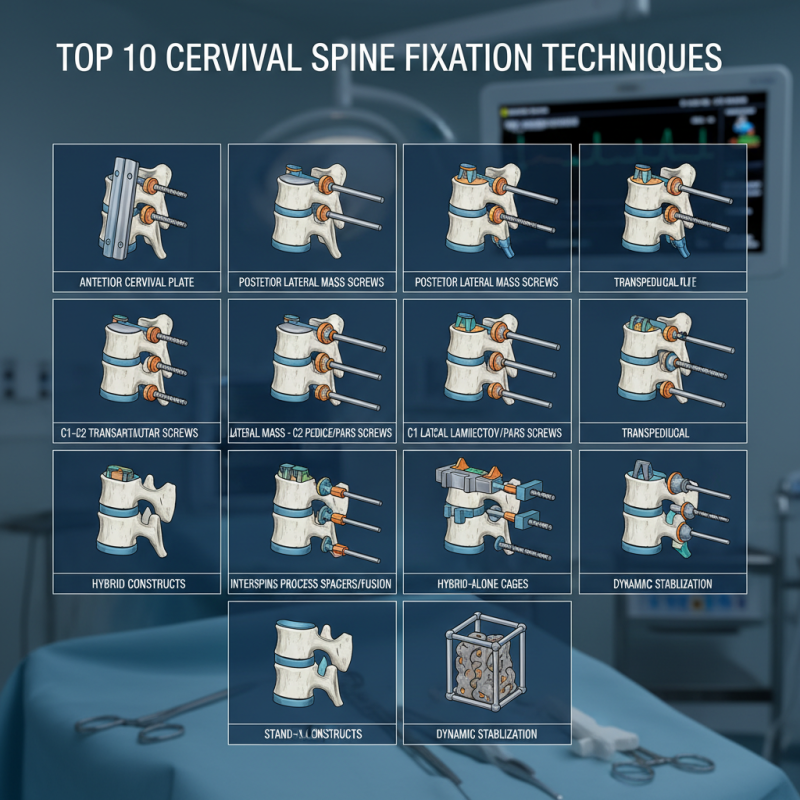
Overview of Cervical Fixation Techniques in Spine Surgery
Cervical fixation techniques play a crucial role in spine surgery, particularly for managing instability and deformities. The foremost approach is
anterior cervical discectomy and fusion (ACDF), noted for its effectiveness in treating cervical disc herniation. Studies reveal that ACDF achieves a fusion rate of over
90%, reaffirming its reliability in clinical settings.
Posterior fixation techniques, such as C1-C2 fusion, are essential for addressing instability in the upper cervical spine. These methods often have higher complication rates and require careful patient selection. Data indicates a complication rate of around
25% in more invasive procedures, which necessitates a thorough evaluation of risks versus benefits.
Innovative techniques, including cervical laminoplasty, focus on decompressing the spinal cord while preserving mobility. Such options are gaining popularity due to their lower complication rates, yet long-term outcomes remain uncertain. The choice of fixation method should be guided by specific patient anatomy and pathology. Each technique presents unique challenges and potentials, underscoring the need for ongoing research and clinician expertise.
Indications and Contraindications for Cervical Fixation Methods

Cervical fixation techniques are vital in treating spinal injuries and disorders. Understanding the indications and contraindications for these methods is crucial for optimal outcomes. Indications include severe cervical instability, trauma, or degenerative diseases. For instance, patients with advanced cervical spondylosis may greatly benefit from these techniques. Surgeons often need to weight the risks and benefits carefully before proceeding.
Contraindications must be considered to avoid complications. Severe osteoporosis can increase the risk of failure. If a patient has a history of infections or tissue necrosis, surgical intervention could pose serious risks. Additionally, patients with significant comorbidities may not tolerate the procedure well. It’s essential for the healthcare team to have thorough discussions with the patient regarding these factors. Doing so helps in making informed decisions and managing expectations effectively. Taking this approach enhances both safety and efficacy in cervical fixation surgeries.
Analysis of Anterior Cervical Discectomy and Fusion (ACDF)
Anterior Cervical Discectomy and Fusion (ACDF) is a common surgery for neck pain. This procedure involves removing herniated discs that press on nerves. Surgeons aim to relieve pain and improve mobility. ACDF can address conditions like cervical disc degeneration effectively.
The process begins with an incision in the front of the neck. Surgeons carefully access the vertebrae. They remove the damaged disc and relieve the pressure on the spinal cord. After the discectomy, they typically insert a bone graft. This graft helps stabilize the spine during the healing process. Patients look forward to reduced pain and improved function.
However, like any surgical technique, ACDF has risks. Complications may include infection, nerve damage, or persistent pain. Each patient's anatomy and condition is unique, so outcomes can vary. Preoperative discussions are essential to set realistic expectations. Understanding these factors contributes to better decision-making about cervical fixation techniques.
Top 10 Cervical Fixation Techniques You Need to Know
| Technique | Surgical Approach | Indication | Recovery Time | Complications |
|---|---|---|---|---|
| Anterior Cervical Discectomy and Fusion (ACDF) | Anterior | Herniated disc, spinal stenosis | 4 to 6 weeks | Infection, nerve damage |
| Posterior Cervical Laminectomy | Posterior | Spinal stenosis, tumors | 6 to 8 weeks | Cerebrospinal fluid leak |
| Cervical Artificial Disc Replacement | Anterior | Degenerative disc disease | 4 to 12 weeks | Device failure, dysphagia |
| Cervical Corpectomy | Anterior | Severe osteophyte formation | 8 to 12 weeks | Fusion failure, infections |
| Lateral Mass Screw Fixation | Posterior | Instability, trauma | 6 to 10 weeks | Neuronal injury, screw misplacement |
| Occipitocervical Fusion | Posterior | Severe instability | 3 to 6 months | Nonunion, infection |
| Transoral Approach | Transoral | Cervical spine tumors | 4 to 8 weeks | Wound complications, infection |
| Minimally Invasive Cervical Surgery | Posterior/Anterior | Herniated disc | 2 to 4 weeks | Recurrence, nerve damage |
| Cervical Plating | Anterior | Stabilization after discectomy | 4 to 8 weeks | Plate breakage, infection |
| Screw-Rod System | Posterior | Cervical instability | 6 to 12 weeks | Hardware failure, infection |
Comparison of Posterior Cervical Fusion Techniques
Posterior cervical fusion techniques are critical in treating various spinal conditions. These techniques aim to stabilize the cervical spine and alleviate pain. Data shows that over 60% of spinal surgeons prefer posterior approaches for certain cases. This preference stems from the technique’s efficiency in accessing the targeted area. Surgeons can better visualize the anatomy, leading to more precise interventions.
One common method involves the use of pedicle screws and rods. This fixation system allows for strong stabilization. Research indicates a success rate of approximately 85% after such procedures. However, complications can arise. Issues like screw misplacement and infection rates are concerns that need addressing. Moreover, a study highlighted that nearly 15% of patients experience some form of postoperative discomfort.
Surgeons must consider various factors when choosing the right technique. Each patient's condition is unique, which complicates decision-making. While posterior cervical fusion can be effective, the variability in individual anatomy presents challenges. Surgeons often reflect on their experiences to improve outcomes and minimize complications.
Top 10 Cervical Fixation Techniques Comparison
Emerging Technologies in Cervical Fixation: Trends and Outcomes
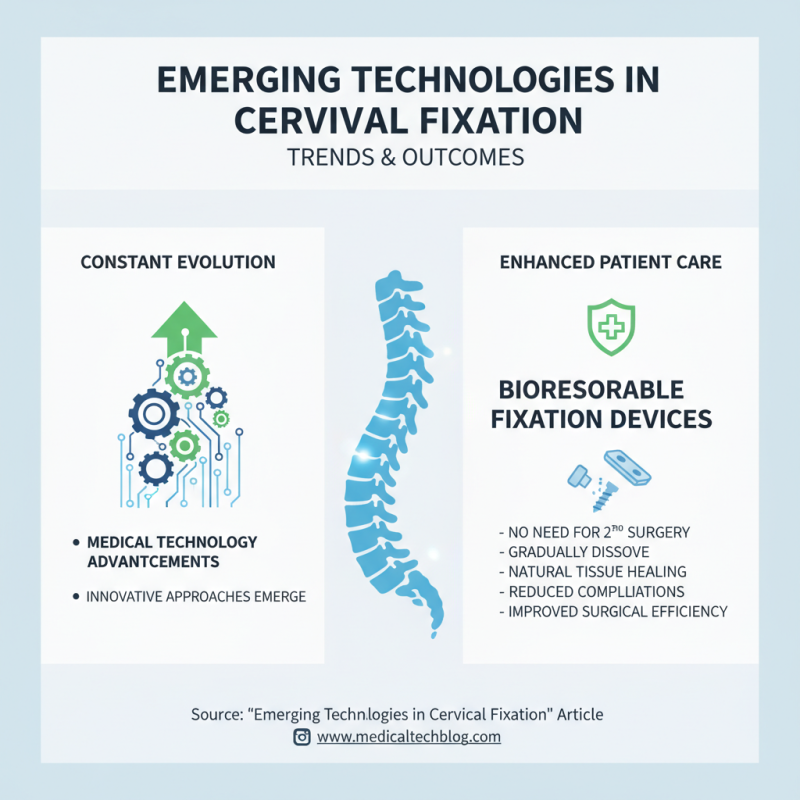
Cervical fixation techniques undergo constant evolution, reflecting advancements in medical technology. Recently, innovative approaches have emerged, enhancing patient outcomes and surgical efficiencies. For instance, bioresorbable fixation devices are gaining traction. They eliminate the need for a second surgery to remove hardware. These devices gradually dissolve, leaving natural tissue to heal without interference.
Robotic-assisted surgery is also noteworthy. This technique offers greater precision in cervical procedures. Surgeons can navigate complex anatomical structures more effectively, reducing the risk of damage. However, the high cost and the learning curve associated with this technology are points of concern. There’s still a debate about its long-term benefits versus traditional methods.
3D printing technology provides individualized fixation solutions. Custom-made implants that fit each patient’s unique anatomy could improve surgical success rates. Yet, this field still faces regulatory challenges and requires more research. There’s a need for ongoing discussions to validate these methods thoroughly. Emerging technologies offer promise but must be approached with caution and diligence in implementation.
Related Posts
-
10 Best Techniques for Posterior Lumbar Interbody Fusion?
-
10 Essential Tips for Choosing Surgical Solutions Inc for Your Needs?
-

2026 How to Understand Disc Fusion for Effective Spine Recovery?
-

How to Choose the Right Screw System for Your Project?
-

Top 10 Surgical Surgeons in China You Should Know About?
-

What is Lateral Interbody Fusion at the 139th Canton Fair?
